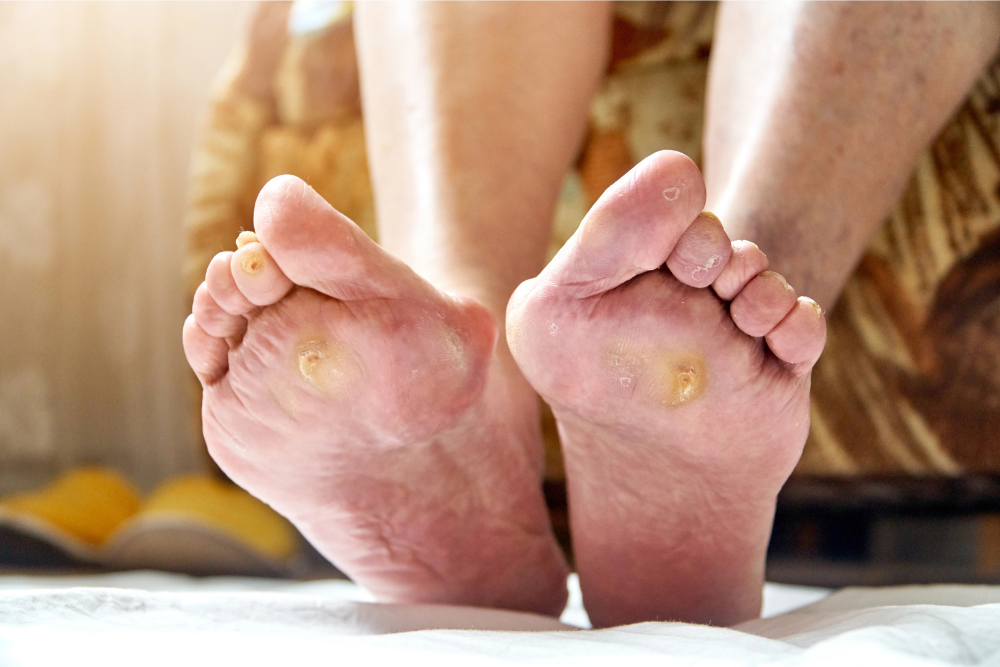
When a patient walks into the office with an open sore on their foot or lower leg, the first thing they usually say is, “It just won’t heal.” From their perspective, it looks like any other wound. It may be red, moist, or slightly swollen. Sometimes it has been there for weeks. What most people do not realize is that not all ulcers are the same, even if they look similar on the surface.
The difference between a diabetic foot ulcer and a venous foot ulcer lies beneath the skin. Both are chronic wounds. Both can linger. Both can become serious if ignored. What truly separates them is why they develop and how they need to be treated. When we clearly understand what sets diabetic and venous ulcers apart, we make better decisions early, and that can change the entire course of healing.
Delaying treatment increases risk. Infection, deeper tissue damage, and prolonged recovery are all more likely when the underlying cause is not addressed early. Choosing the correct foot ulcer treatment depends on making the right diagnosis from the start.
A diabetic foot ulcer develops as a complication of long-standing or poorly managed diabetes. Over time, elevated blood sugar affects small blood vessels and peripheral nerves, particularly in the feet. This nerve damage, known as neuropathy, reduces the ability to feel pain, pressure, or temperature changes.
In every day life, that loss of sensation makes the foot more prone to injury. A blister from a tight shoe, a small cut, or a call us under the ball of the foot may go unnoticed. Because the patient does not feel discomfort, pressure continues on the same area. Eventually, the skin breaks down and a diabetic foot ulcer forms.
These ulcers most commonly appear on weight-bearing areas, such as the toes, the bottom of the foot, or the heel. That location is a key factor when identifying diabetic foot ulcers from venous ulcers. Diabetic wounds are strongly linked to pressure and repetitive stress.
Often, the surrounding skin appears thickened or callused. The wound itself may look deeper than expected. Surprisingly, many patients report little pain. The absence of discomfort is not reassuring. In fact, it is one of the reasons diabetic foot ulcers can progress quickly without drawing attention.
Effective diabetic foot care focuses on prevention and pressure relief. Blood sugar management plays a major role in healing. Without stable glucose levels, the body struggles to repair tissue and fight infection. Preventing diabetic foot ulcers requires daily foot inspections, appropriate footwear, and routine podiatric evaluations.
Also Read: Wound Healing and Diabetes: When to See a Diabetic Foot Specialist
A venous foot ulcer forms for a completely different reason. Instead of nerve damage, the issue lies in the veins of the lower leg. When the valves inside those veins weaken, blood does not flow back toward the heart efficiently. It pools in the lower extremities, increasing pressure in the surrounding tissues.
Patients often notice swelling and discomfort that worsens throughout the day. They may describe a feeling of heaviness or aching in the lower leg. Over time, the skin changes. It can become darker in color, irritated, or shiny. The tissue grows fragile due to chronic inflammation and fluid build up.
Eventually, even minor trauma can lead to skin breakdown. A venous foot ulcer usually appears around the inner ankle or lower leg rather than on the bottom of the foot. That location provides one of the clearest clues in distinguishing between these two conditions.
Pain patterns differ as well. Venous ulcers often cause discomfort that improves when the leg is elevated. This positional relief suggests that circulation and fluid return are part of the problem. In contrast, diabetic ulcers may cause minimal pain because neuropathy dulls sensation.
Venous ulcer care centers on improving blood return and reducing swelling. Without correcting the underlying vein dysfunction, healing remains slow, and recurrence is common.
Also Read: Early Warning Signs of Venous Stasis Ulcers You Shouldn’t Ignore
Diabetic foot ulcers tend to form at pressure points, along the sole or on the toes, areas that absorb force every time you walk. Venous foot ulcers, on the other hand, are much more likely to appear around the ankle or lower leg, where fluid tends to collect.
Beyond location, the root cause tells an even clearer story. Diabetic ulcers are typically driven by nerve damage and long-term metabolic changes. Venous ulcers develop when veins fail to efficiently circulate blood, leading to fluid buildup and chronic inflammation.
Pain patterns also help guide us. Many diabetic wounds cause surprisingly little discomfort because sensation is reduced. Venous ulcers often ache, especially after prolonged standing, and patients frequently tell me the discomfort improves when they elevate the leg.
Even the skin around the wound gives clues. Thick callus formation suggests repeated pressure in a neuropathic foot. Swelling and darkened skin point toward venous disease.
When you put all of these pieces together, the diagnosis becomes much clearer, and so does the direction of treatment.
Treatment for diabetic and venous foot ulcers must target the underlying cause, not just the visible wound.
For diabetic foot ulcers, offloading is critical. This means reducing pressure on the affected area through specialized footwear, casts, or custom devices. Continued pressure prevents healing, no matter how advanced the dressing may be.
At the same time, glucose control is essential. High blood sugar impairs immune response and slows tissue repair. Diabetic foot care extends beyond the wound itself. It requires coordination with overall diabetes management.
Venous ulcers require a different approach. Compression therapy plays a central role. Graduated compression supports blood flow back toward the heart and reduces swelling. Leg elevation several times a day further assists circulation.
Using the wrong strategy can delay healing. Applying compression without proper evaluation of circulation may be unsafe in certain cases. Not relieving pressure for a diabetic ulcer leads to continued tissue breakdown. A foot ulcer specialist evaluates circulation, nerve function, and wound characteristics before deciding on a plan.
If you have a wound that looks the same today as it did two weeks ago, that is a sign to get it checked. Foot ulcers rarely heal on their own without addressing the underlying cause. The longer you wait, the greater the risk of infection or deeper tissue involvement.
Pay attention to changes like persistent drainage, spreading redness, warmth, odor, or an increase in size. In people with diabetes, especially, small changes can escalate faster than expected. Acting early almost always means a simpler treatment plan and a better outcome.
A thorough evaluation begins with a detailed medical history. We ask about diabetes control, circulation issues, prior ulcers, and daily activity levels.
Next comes a focused examination. Circulation is assessed through pulse checks and sometimes, non invasive testing. Nerve sensation is evaluated to determine the presence and severity of neuropathy.
The ulcer itself is measured carefully. Depth, tissue quality, drainage, and surrounding skin changes are documented. Imaging may be considered if deeper structures are involved.
The treatment plan is tailored to the patient’s medical history, physical findings, and wound assessment. Foot wound care may include debridement, specialized dressings, off loading devices, compression therapy, or referral for vascular assessment. Treatment for diabetic and venous foot ulcers must always reflect the specific diagnosis.
Also Read: Your Guide to Podiatry: Foot & Ankle Conditions, Treatments, and When to Seek Care
Prevention requires consistency and awareness. For individuals with diabetes, daily foot checks help identify redness, blisters, or call us formation before they become ulcers. Preventing diabetic foot ulcers is often easier than managing advanced wounds.
If you live with diabetes, think of those daily checks as a simple habit that protects you long term. Taking a few quiet minutes to look at the tops and bottoms of your feet, and between your toes, can help you catch subtle changes before they turn into open wounds. Keeping your blood sugar within a healthy range does more than support overall wellness. It protects nerve function and gives your body a better chance to heal after minor injuries. The shoes you choose matter as well. Properly fitted footwear reduces pressure and friction invulnerable areas, especially along the toes and the ball of the foot.
If vein disease is part of your medical picture, the focus shifts slightly. In that case, swelling control becomes central to both healing and prevention. Consistent use of compression stockings, regular movement throughout the day, and elevating your legs when possible can significantly reduce fluid build up and lower the risk of recurrence. Follow-up visits with a podiatric provider help reinforce these strategies. Often, small adjustments in footwear, skin care, or compression level make a meaningful difference over time.
Foot ulcers are not just minor wounds. They signal deeper issues involving circulation or nerve function. The right diagnosis protects mobility and overall health.
If you are dealing with non-healing foot wounds or need clarity about the difference between diabetic foot ulcers and venous foot ulcers, schedule an evaluation with Advanced Foot and Ankle Specialists. Early, specialized care can significantly improve healing and prevent complications.
